Can you bill modifier 59 and 51 together?
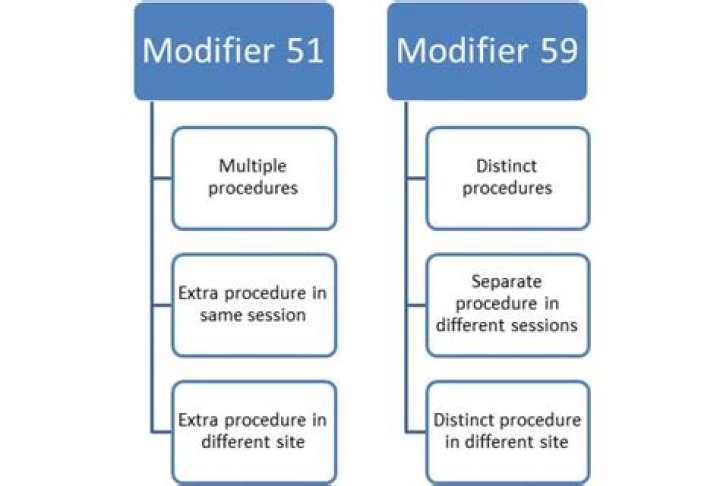
There are two modifiers commonly used in surgical specialties when billing two or more procedures at the same encounter. Appending the correct modifier increases the likelihood that the claim will be paid the first time, correctly. Never use both modifier 51 and 59 on a single procedure code.
Can modifier 59 be used twice?
If the 59 modifier is appended to either code, they will both be allowed on the claim separately. However, the 59 modifier should only be added if the two procedures are performed in distinctly separate 15 minute intervals. If the codes were performed on the same nerve, then the 59 modifier should not be used.
Can 97530 and 97110 be billed together?
Bottom line: when 97530 and one of the physical therapy evaluation codes are billed together on the same day for the same patient, the evaluation code will be denied. Answer: CPT code 97110 is a therapeutic procedure, on one or more areas, each lasting 15 minutes.
What is the 59 modifier used for?
Modifier 59 is used to identify procedures/services, other than E/M services, that are not normally reported together, but are appropriate under the circumstances.
What replaced modifier 59?
Medicare recently announced they’ve established four new modifiers – XE, XS, XP, and XU – that may be used in lieu of modifier 59. The codes are more specific and become effective January 1, 2015.
Can 97535 and 97530 be billed together?
Some other therapy code combinations that require Modifier 59 to enable the codes to be billed individually on the same day are: 97530 (Therapeutic Activity) and 97535 (ADL) 97140 (Manual Therapy) and 97530 (Therapeutic Activity) 97542 (Wheelchair Mobility) and 97530 (Therapeutic Activity)
What is the 58 modifier?
Modifier 58 is defined as a staged or related procedure performed during the postoperative period of the first procedure by the same physician. A new postoperative period begins when the staged procedure is billed.
Can 97164 and 97140 be billed together?
As of January 1, 2020, the National Correct Coding Initiative (NCCI) has stated that if you bill an initial evaluation code (97161, 97162, 97163) or a re-evaluation code (97164) on the same date of service for the same patient as CPT code 97140 (Manual therapy), you MUST affix modifier 59 to 97140 in order to receive …
What is EY modifier?
Please remember that if you submit a claim to Medicare and specified requirements for an order are not met, you must append modifier EY (“No physician or other licensed health care provider order for this item or service”) to the claim line. …
What is the Xu modifier?
Modifier Code XU This modifier is used to identify “unusual non-overlapping services, the use of a service that is distinct because it does not overlap usual components of the main service”.
Can modifiers 24 and 57 be used together?
E/M service resulting in initial decision to perform major surgery is furnished during post-operative period of another unrelated procedure, then the E/M service must be billed with both the 24 and 57 modifiers.
What is a 57 modifier?
Modifier 57 is used to indicate an Evaluation and Management (E/M) service resulted in the initial decision to perform surgery either the day before a major surgery (90 day global) or the day of a major surgery.



