science /
Why are colonoscopies not recommended after age 75?
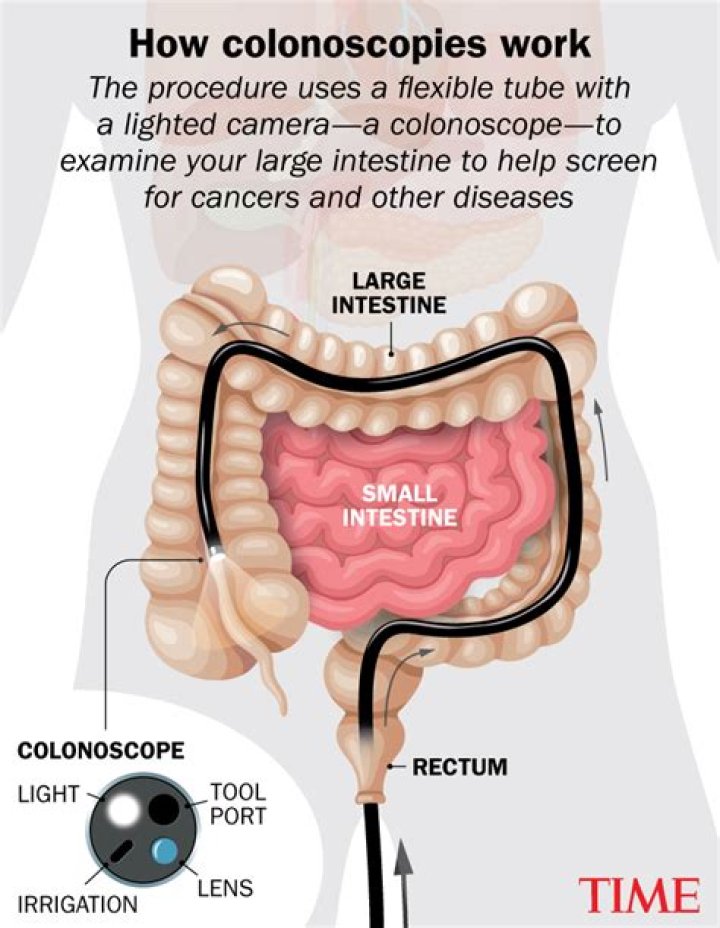
“There are risks involved with colonoscopy, such as bleeding and perforation of the colon, and also risks involved with the preparation, especially in older people,” Dr.
Can you have a colonoscopy after 75 years old?
There's no upper age limit for colon cancer screening. But most medical organizations in the United States agree that the benefits of screening decline after age 75 for most people and there's little evidence to support continuing screening after age 85.Does Medicare cover colonoscopy after age 75?
Screening guidelines from the U.S. Preventive Services Task Force recommend screening for colon cancer with any method, including colonoscopy, from age 50 to 75. Medicare reimburses colonoscopy, regardless of age.How often should a 75 year old have a colonoscopy?
For those opting to undergo colonoscopies (other screening options include a fecal occult blood test and flexible sigmoidoscopy), the procedure should be done every 10 years, and is not needed after age 75. Colon cancer tends to progress slowly, Sheffield said, so early detection is less likely to benefit older adults.Is 80 too old for colonoscopy?
Conclusions: Colonoscopy in patients 80 or more years of age is safe, effective, and has a high diagnostic yield. Procedure times are slightly longer, and the ileoscopy rate is lower in this age group.Colonoscopies not always necessary for older adults: Study
At what age can colonoscopies be stopped?
The guidelines: recommend screening for colorectal cancer using fecal occult blood testing, sigmoidoscopy, or colonoscopy in adults, beginning at age 50 years and continuing until age 75. recommend against routine screening for colorectal cancer in adults age 76 to 85 years.Is there an alternative to colonoscopy?
Alternatives to colonoscopy include sigmoidoscopy, which is a less invasive form of colonoscopy, and noninvasive methods, such as stool sample testing.Can I do cologuard instead of colonoscopy?
The majority of large precancerous polyps cannot be detected with Cologuard. This may give patients a false sense that they are preventing colon cancer by taking the Cologuard test. In short, there is no true replacement for a colonoscopy.How do you prevent colon polyps from coming back?
Research suggests that making the following changes may have health benefits and may lower your chances of developing colon polyps:
- eating more fruits, vegetables, and other foods with fiber , such as beans and bran cereal.
- losing weight if you're overweight and not gaining weight if you're already at a healthy weight.
What is the average number of polyps removed in a colonoscopy?
The average BBPS was 7.2 ± 1.5, and adequate bowel preparation (a score of ≥ 2 in each segment of the colon) was achieved in 88.2 % of patients (1709 /1937). The mean number of endoscopically detected polyps per procedure was 1.5 ± 2.3 (95 % confidence interval [CI] 1.4 – 1.6).How often should you have a colonoscopy after 70?
Groups like the U.S. Preventive Services Task Force (USPSTF), the American Cancer Society and the American College of Gastroenterology agree that routine screening colonoscopies should be carried out every 10 years starting at age 50.Does Medicare pay for mammograms after age 75?
Does Medicare pay for mammograms after age 75? Part B continues to cover screening and diagnostic mammograms for women in their late 70s. Medicare pays the full cost of testing annually, and 80% of the cost of diagnostic mammograms. About 14% of breast cancer diagnoses occur in women aged 75-84.How Much Does Medicare pay towards a colonoscopy?
Original Medicare pays the full cost of a colonoscopy if a medical provider who accepts Medicare rates does the procedure. However, if a polyp is found and removed during the colonoscopy, the procedure is considered diagnostic rather than preventive and you likely will owe 20 percent of the Medicare-approved fee.Does a 75 year old woman need a Pap smear?
Pap smear.The USPSTF recommends against screening women over age 65 who have had normal Pap smears in "adequate recent screenings" and aren't otherwise at high risk for cervical cancer.